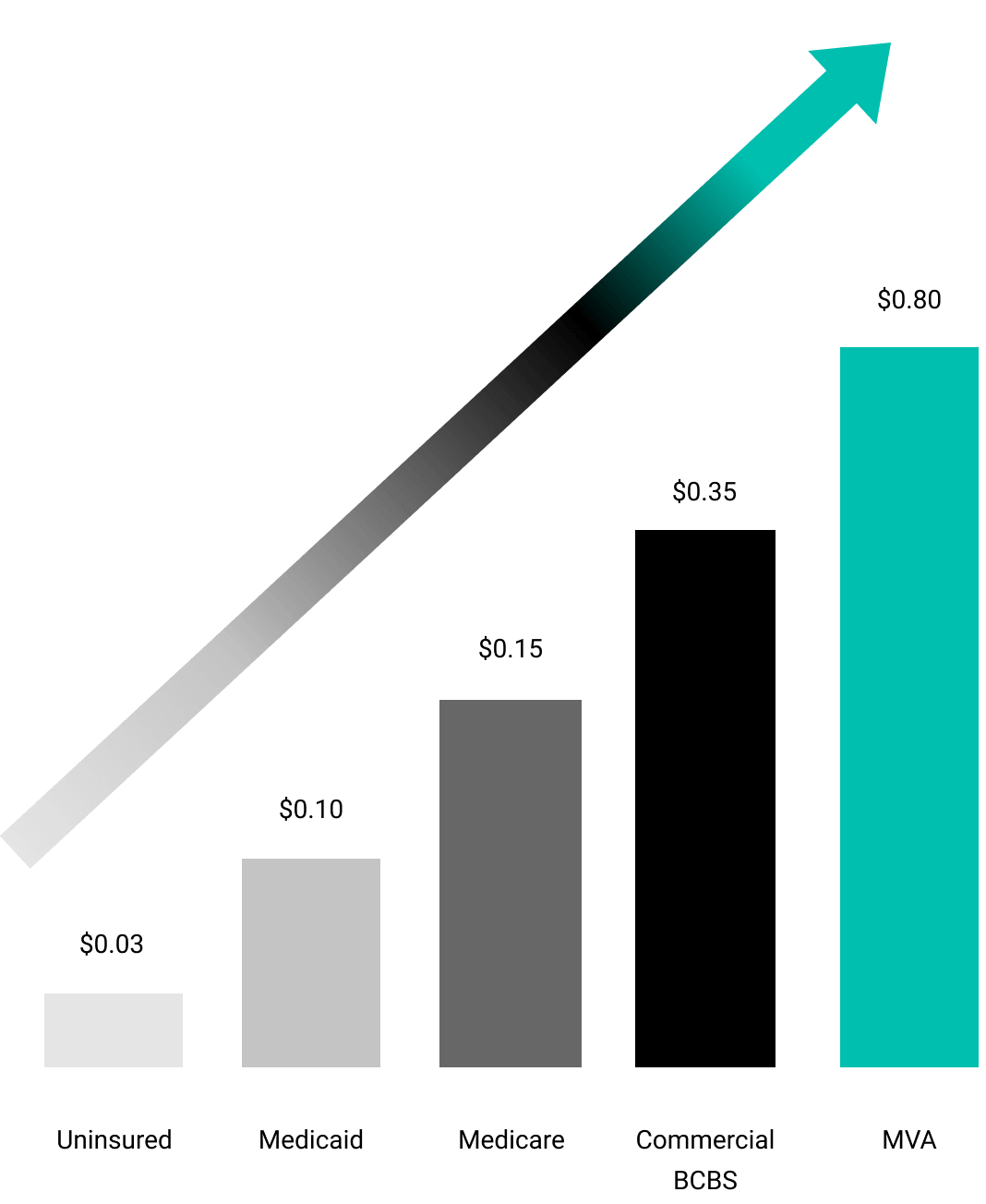
Hospitals, physician groups and other providers routinely miss out on a portion of third-party payments from commercial insurance carriers and government aid.
Medlytix® helps healthcare providers identify and capture these funds, potentially netting millions of dollars.
Advanced Revenue Cycle Solutions
| Patient Population | Insurance Identification and COB | Deductible Monitoring | Predictive Analytics |
|---|---|---|---|
| Uninsured | |||
| Medicaid | |||
| Medicare | |||
| Commercial/BCBS | |||
| TPL-MVA/WC |